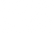
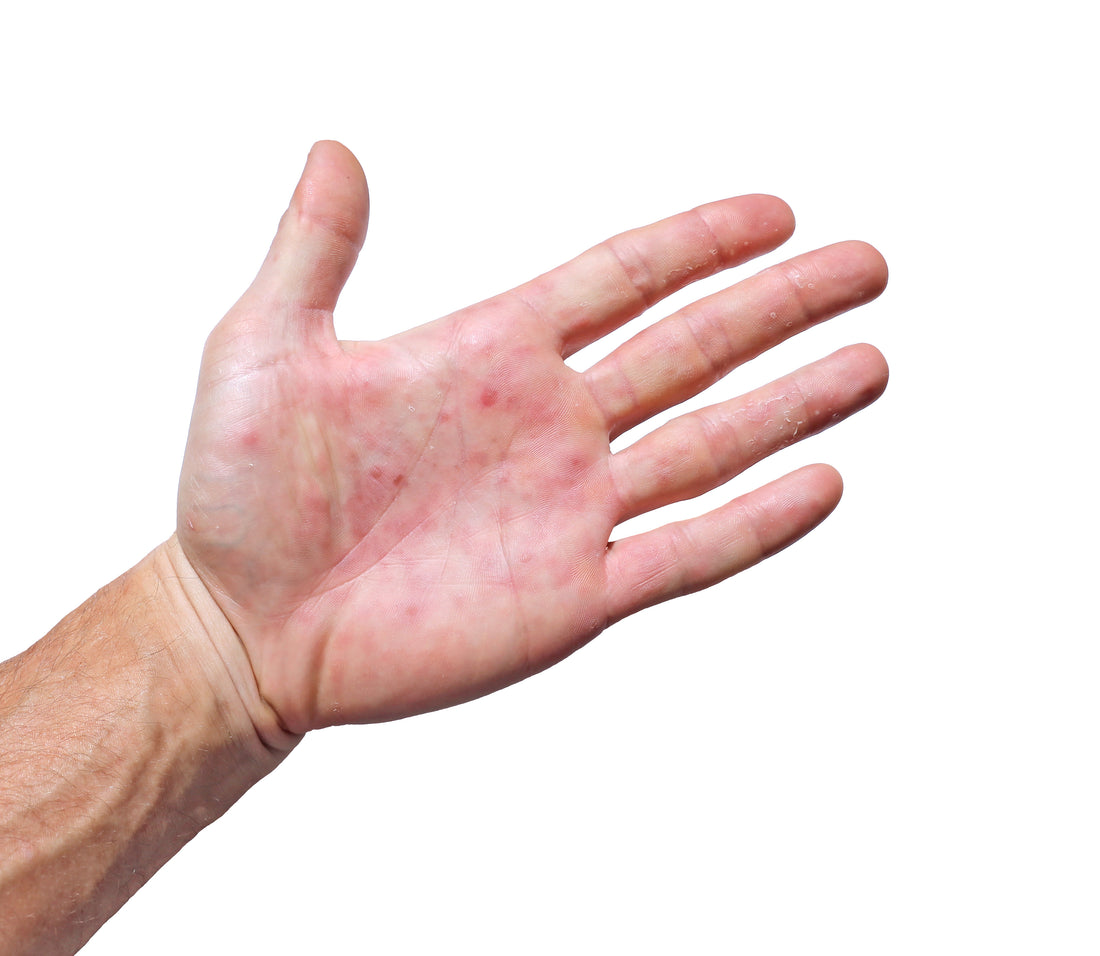
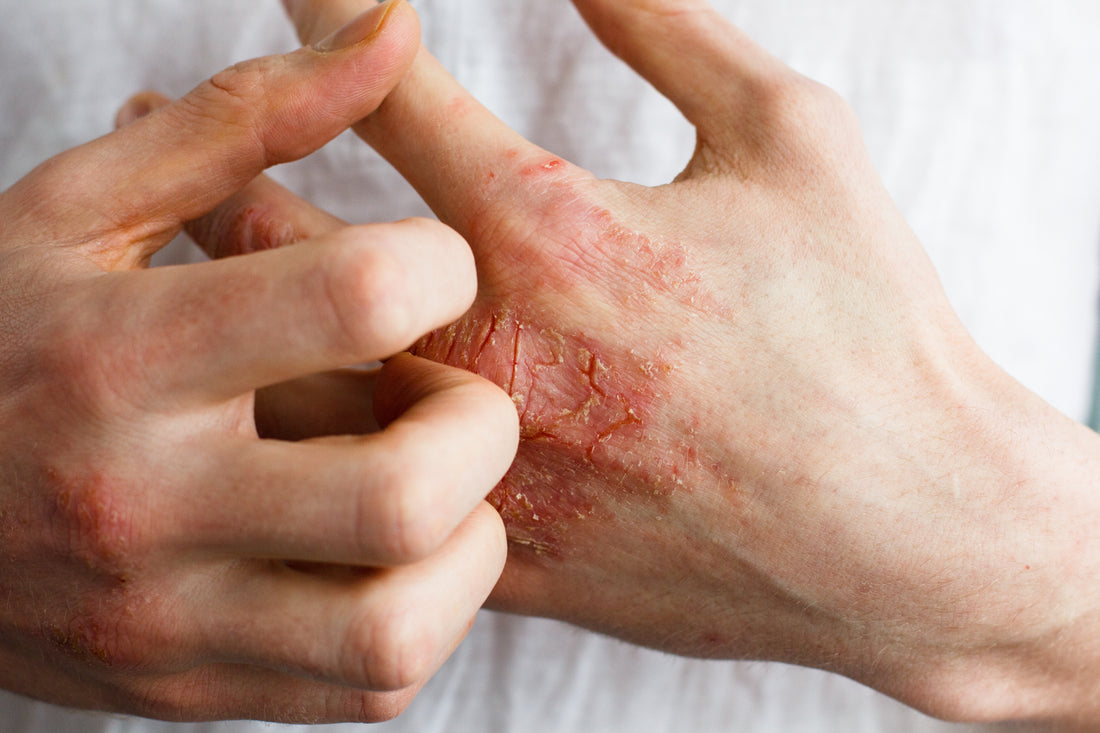
Eczema, also known as atopic dermatitis, is a chronic skin condition that typically begins in childhood but can affect people of all ages. The exact cause of eczema is not fully understood, but it is believed to result from a combination of genetic and environmental factors.
Genetic predisposition plays a significant role in the development of eczema. People with a family history of eczema, asthma, or allergies are more likely to develop the condition. Certain gene mutations are associated with a defective skin barrier function, which makes the skin more susceptible to irritants, allergens, and moisture loss.

Environmental factors also contribute to the onset of eczema. These include:
- Allergens: Exposure to certain substances can trigger or worsen eczema symptoms. Common allergens include dust mites, pet dander, pollen, mold, and certain foods.
- Irritants: Everyday substances can irritate the skin and lead to eczema flare-ups. These irritants may include soaps, detergents, shampoos, fragrances, harsh chemicals, and even some fabrics.
- Dry skin: Individuals with eczema often have a compromised skin barrier, which allows moisture to escape and makes the skin dry and itchy. Dry skin can further aggravate eczema symptoms and trigger flare-ups.
- Climate: Extreme temperatures, high or low humidity levels, and changes in weather conditions can affect the skin and lead to eczema flare-ups.
- Stress: Emotional stress and anxiety can contribute to the development or worsening of eczema symptoms. Stress can weaken the immune system and make the skin more reactive.
It's important to note that while these factors can trigger or exacerbate eczema, the condition is not contagious. Eczema is a result of a complex interplay between genetic and environmental factors, and the exact triggers may vary from person to person. If you suspect you have eczema or are concerned about a skin condition, it's best to consult a healthcare professional or dermatologist for an accurate diagnosis and appropriate treatment.
The allergic march, also known as the atopic march, refers to the natural progression of allergic diseases in some individuals, particularly children. It describes the sequential development of different allergic conditions over time. The typical pattern of the allergic march begins with eczema (atopic dermatitis) in infancy, followed by food allergies, allergic rhinitis (hay fever), and asthma later in childhood.
The exact cause of the allergic march is not fully understood, but it is believed to be influenced by a combination of genetic predisposition and environmental factors. Here's a general overview of how the allergic march starts in children:
- Eczema (Atopic Dermatitis): Eczema often appears in infancy, typically before the age of five. Genetic factors play a significant role in the development of eczema, and children with a family history of eczema, asthma, or allergies are more prone to developing it. Environmental factors like irritants, allergens, dry skin, and changes in temperature can trigger eczema symptoms.
- Food Allergies: Some children with eczema may develop food allergies as part of the allergic march. Common food allergens include cow's milk, eggs, peanuts, tree nuts, soy, wheat, and shellfish. The exact relationship between eczema and food allergies is not fully understood, but it is believed that the compromised skin barrier in eczema patients allows allergens to penetrate more easily, leading to sensitization and allergic reactions.
- Allergic Rhinitis (Hay Fever): Allergic rhinitis typically manifests as sneezing, itching, nasal congestion, and watery eyes in response to allergens like pollen, dust mites, or pet dander. Children who have had eczema or food allergies may develop allergic rhinitis later in childhood. It is thought that the immune system becomes sensitized to various allergens, leading to an allergic response in the respiratory system.
- Asthma: Asthma is a chronic respiratory condition characterized by inflammation and narrowing of the airways, leading to breathing difficulties, coughing, wheezing, and chest tightness. Children with a history of eczema, food allergies, or allergic rhinitis are at an increased risk of developing asthma. The progression from allergic rhinitis to asthma may occur due to shared underlying mechanisms and inflammation in the airways.
It's important to note that not all individuals follow the exact sequence of the allergic march, and the severity and progression of allergic conditions can vary. While the allergic march provides a general framework, each person's experience with allergic diseases can be unique. Early identification, appropriate management, and allergen avoidance under the guidance of healthcare professionals can help in minimizing the impact of the allergic march and improving quality of life for affected individuals.